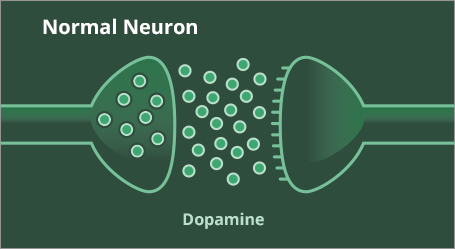
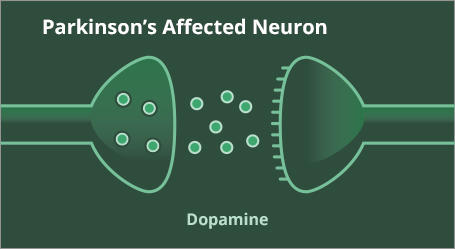
Parkinson’s disease (PD) is a multisystem disorder typically defined by a progressive loss of dopaminergic neurons in the substantia nigra.1,2 By the time of diagnosis, individuals have lost a significant number of dopaminergic neurons—evidence suggests 60-80% of dopaminergic neurons degenerate before clinical features emerge.23 As PD progresses, neurodegeneration continues, with further loss of dopaminergic neurons and dopamine.2 The progression of disease reduces the brain’s ability to store and release dopamine when it is needed.2,3
The characteristic motor symptoms of Parkinson's disease are bradykinesia, tremor and rigidity, all of which are related to the degeneration of dopaminergic neurons in the substantia nigra. However, these symptoms are only one aspect of this multifaceted and complex disorder. It is now suggested that Parkinson's related degeneration is widespread in both the central and peripheral nervous systems.1
Evidence is mounting that many non-nigral sites produce a number of clinical signs and symptoms of Parkinson’s disease.1